
Arine illuminates hidden opportunities to reduce costs by addressing medication issues for your most challenging patients, at a greater velocity than ever before.
We help you intervene quickly so you can improve care and your bottom line.
Identifying people most at risk for medication-related problems and intervening rapidly, with the right care, helps reduce costly interventions. Traditional care management solutions do not leverage medications – one of our most crucial tools – to drive the urgent improvements in care that are needed.
By identifying hidden individuals at increased risk of medication-related problems, we can prevent serious consequences from occurring and reduce the clinical and cost ramifications. This means that your team can reduce hospitalizations by >40% within six months, contributing to cost of care savings more than 10%.
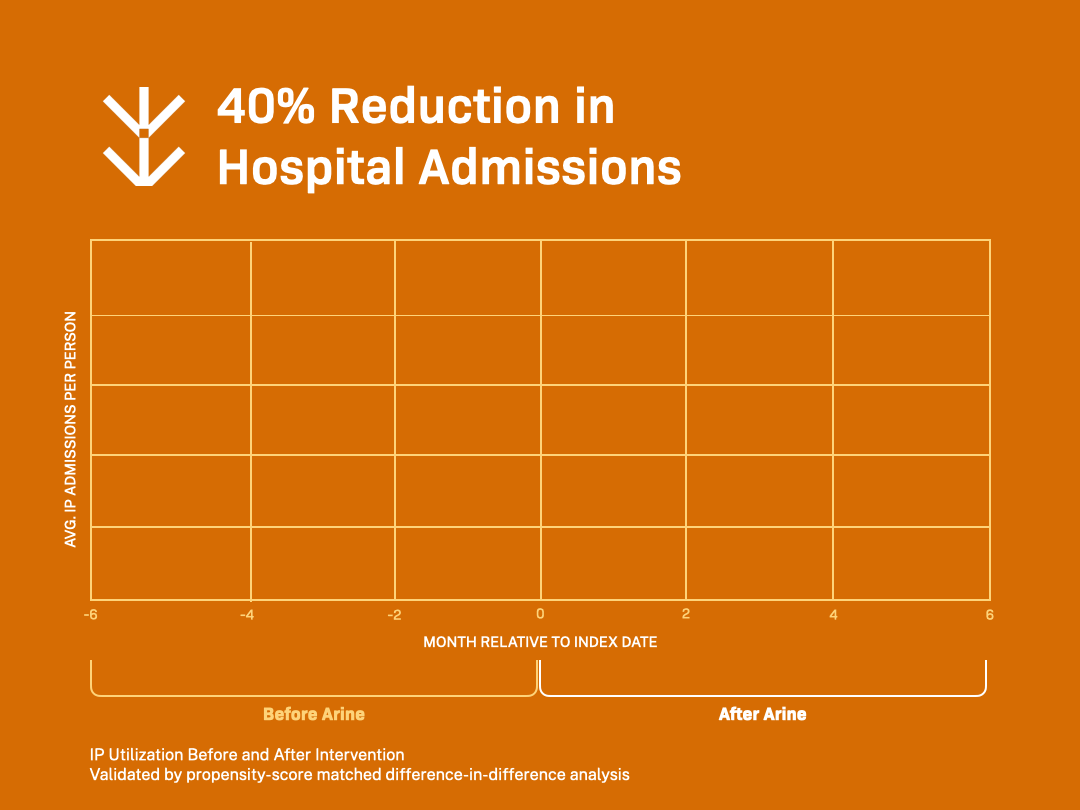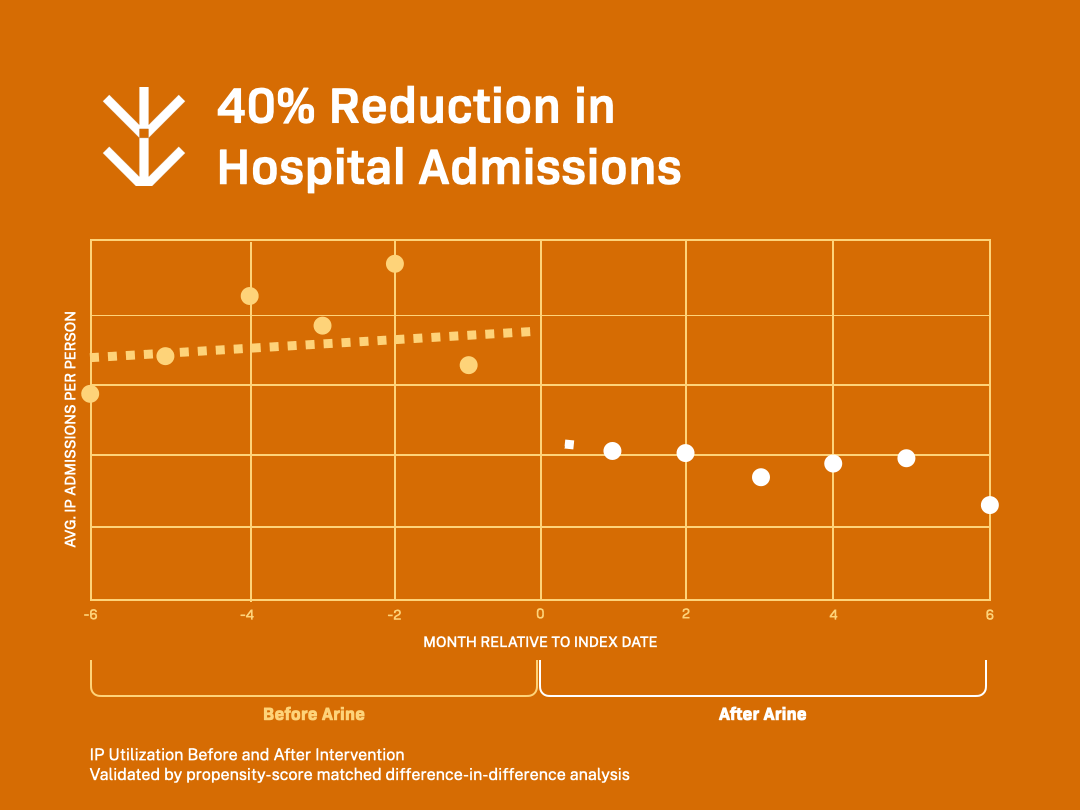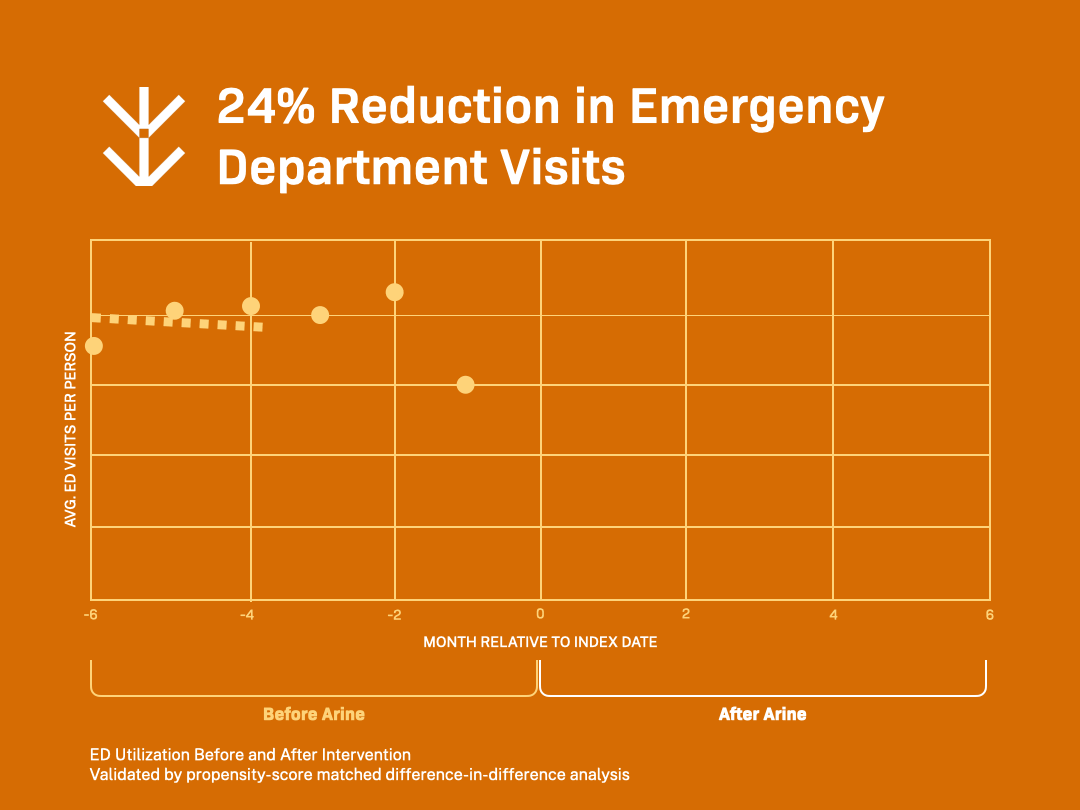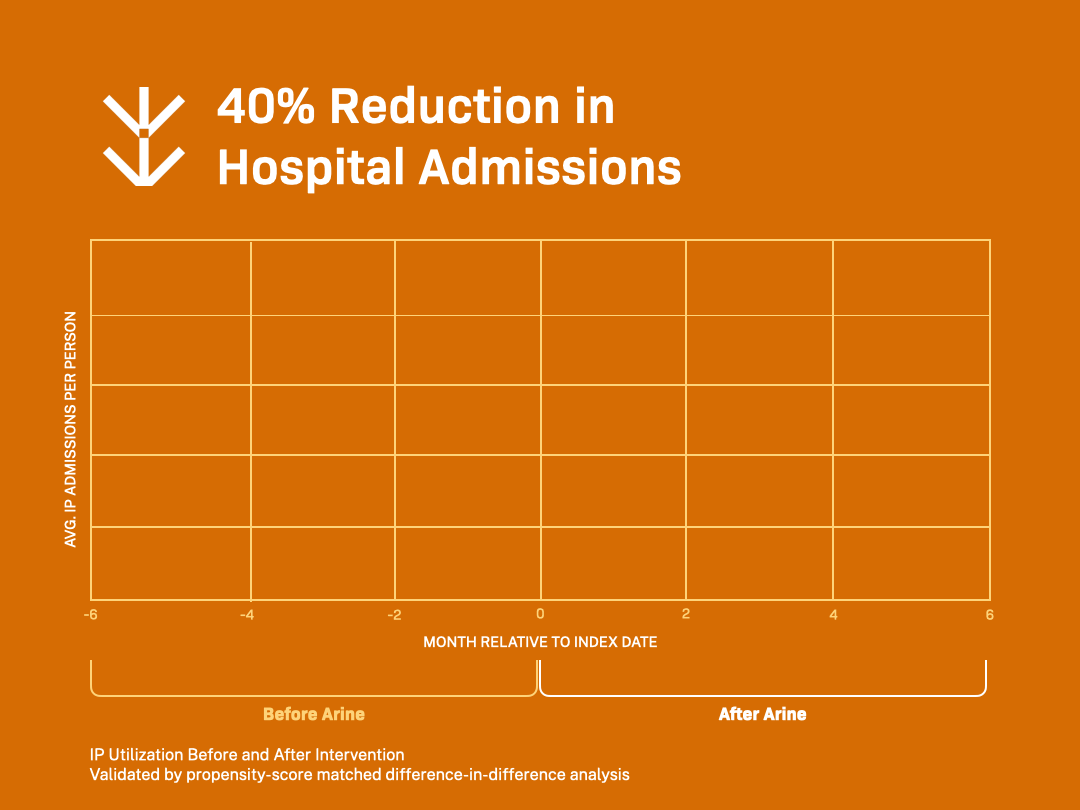
Reduced Total Cost of Care with Arine
Reduced Hospital Readmissions with Arine
Increased Specialty Care Plans Created





Arine's AI models, each leveraging hundreds of data features, find the individuals most at risk for near-term costly interventions.
Our platform integrates broad data sets to reveal members of your population with impending medication-related problems including drug/drug interactions, underutilization of care, and incorrect dosing.

Arine’s platform supports immediate, impactful interventions for each individual based on their specific needs, empowering you to help more members.
Arine enables quick outreach through automatically generated personalized care plans. Our workflow engines ensure care teams operate at maximum efficiency, assigning tasks to the right care team member at the right time.

Arine instills trust and commitment from providers and patients so recommendations are promptly implemented.
Our patient materials and provider communications address the specific needs of each audience, leading to >50% clinician acceptance rates.

Arine dynamically updates its patient profiles and recommendations to ensure relevancy and impact.
Our AI learns from your data to promptly update recommendations and further optimize care. Our live dashboards enable your team to continually monitor performance and intervene as needed.
Arine’s platform gave clinicians actionable insights that enabled them to meet the needs of each individual member. This approach allowed us to efficiently scale care, optimize medication therapy, improve health and economic outcomes, and reduce barriers for vulnerable members.
Senior Pharmacy Director, Oklahoma Health Care Authority
Learn how Oklahoma Health Care Authority improved the health of their Medicaid population while also driving cost savings within six months.

Health plans and patients invest significant time and resources on specialty drugs.
However, their benefits can quickly fade, or not be realized, if patients are not effectively managed on these important medications.
Arine considers each patient’s full profile, taking into account clinical, behavioral, and social considerations, to ensure any changes to their regimen are clinically indicated. We can help your team monitor patient experiences and outcomes, so that side effects are managed and escalations in therapy occur as appropriate.
This means that your patients are more likely to be successful on therapies and you achieve the outcomes you expect and are paying for.
Arine identifies opportunities from detailed patient profiles based on clinical, social, and behavioral data.
Arine automatically generates impactful prescriber communications and patient care plans so your team can support more members more quickly.
Arine continually measures outcomes, refining recommendations so you can realize benefits more rapidly.
Uncover hidden opportunities to immediately support patients at higher risk and reduce cost of care.